INTRODUCTION
Brachytherapy using I-125 and a variety of other isotopes in removable episcleral plaques is often used in the treatment of ophthalmic tumors (2, 6, 8, 16, 20, 21, 23). Plaque based brachytherapy permits higher tumor doses with greater sparing of non-involved tissues compared to x-ray teletherapy. Plaque therapy is more accessible, and less expensive, time consuming, and labor intensive than heavy charged particle teletherapy (4, 9, 10). A Phase III national study, the Collaborative Ocular Melanoma Study (COMS), is currently comparing the efficacy of plaque brachytherapy for moderately large tumors (3 to 8 mm height) versus enucleation.
Ophthalmic plaques fall into two general catagories: (a) those that are supplied as ophthalmic applicators (2, 3, 5, 16, 23) with relatively long lived isotopes (Co-60 and Ru-106) and (b) those into which sealed radioisotope sources (Ir-192 or I-125) are temporarily inserted (1, 6, 12, 17, 21). The COMS participants use five standard sizes of sealed source plaques (6, 12). These plaques consist of a bowl shaped outer shell made of a gold alloy and a seed carrier insert made of silicone rubber. The silicone insert simplifies seed installation and offsets the seeds by 1 mm from the scleral surface. The gold shell is a symmetrical segment of a spherical surface which is terminated by a cylindrical lip of about 3 min height. The lip holds the silicone insert and provides limited collimation of the photon flux from the plaque. Projecting from the lip are small eyelets which are used to suture the plaque to the sclera. Plaque diameters of 12 mm, 14 mm, 16 mm, 18 mm and 20 mm, measured at the lip, are available (Trachsel Dental Studio, Rochester, Minnesota, USA.). I-125 is the isotope designated (6) by the COMS. Sealed I-125 sources in the form of seeds (Model 6711, 3M Corp., Medical Products Div., St. Paul, MN, USA.) are placed into the slots of the seed carrier, which is then inserted into the gold shell. The COMS plaques are pictured in Figure 1. Many alternatives to the COMS plaques have been reported in the literature for I-125 and Ir-192 seeds. Some of these alternatives permit asymmetrical designs (17, 21) and/or the incorporation of hyperthermia (1, 7). Asymmetrical plaques combined with a low energy isotope are particularly suited to treating tumors in close proximity to the optic nerve or macula.

|
Fig. 1. The plaques used in the Collaborative Ocular Melanoma Study (COMS) have diameters ranging from 12 to 20 mm, and lip heights from 2.5 to 3.3 mm. I-125 seeds are loaded into a silicon carrier which is then inserted into the 0.5 min thick gold alloy shell. The silicon carrier offsets the seeds by 1 mm from the scleral surface. Six suture eyelets project from the lip of a plaque at 30° intervals.
|
While initial tumor responses following ophthalmic radiotherapy have been good, late complications continue to be reported. Complications include scleral necrosis, macular edema, cataract, neovascular glaucoma and vasculopathy of the retina and optic nerve (5, 8, 11, 20, 22). It is of interest to obtain precise dosimetry in the immediate vicinity of ophthalmic plaques to determine if such data will correlate strongly with complications of treatment.
In this report we describe an ophthalmic plaque dosimetry program, implemented on a microcomputer workstation, which uses a highly interactive 3-dimensional graphics interface. The program provides detailed dosimetry for the COMS plaques, and has general application to all seed carrying plaques. In particular, isotope decay, source anisotropy, inhomogeneous scatter, and collimation provided by the lip at the edge of a plaque are accounted for.
METHODS AND MATERIALS
Computer system
The dosimetry program was originally developed on a personal computer (PC-XT, IBM Corporation, Boca Raton, FL, USA.), and subsequently adapted to the multiwindow environment of an inexpensive workstation (Macintosh II, Apple Computer Inc., Sunnyvale, CA, USA.) The original version was coded (Turbo Pascal 3.0, 8087 version, Borland International, Scotts Valley, CA, USA.) using a commercial graphics primitives (Halo™, Media Cybernetics, VA, USA.) library. The current version is coded (LightspeedC 3.0, Symantec, Bedford, MA, USA.) using the workstation's graphics "toolbox". The workstation displays 640 X 480 pixels at 72 ppi and 256 colors per pixel. The color graphics in this article were photographed from the workstation's video monitor.
Plaque files
|
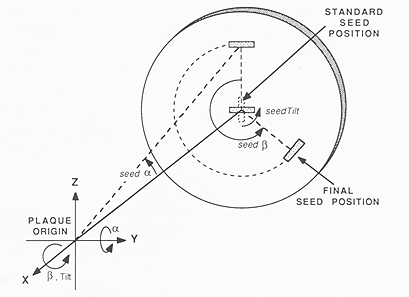
Fig. 2. The origin of a plaque's coordinate system is the center of the sphere to which it conforms. The position and orientation of a slot is specified by 3 angles which describe the displacement from a standard position and orientation. The seed is first rotated about the x-axis by seedTilt, then rotated about the y-axis by seed α, and finally rotated about the x-axis once again by seed β.
|
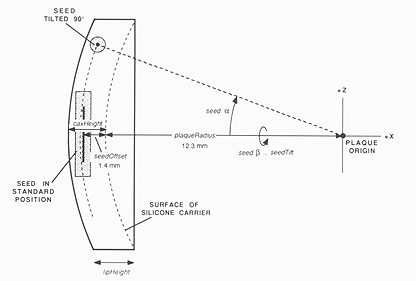
Digitizing the coordinates of individual seeds for dosimetric purposes is laborious and prone to inaccuracy. This task can be simplified by observing that the seeds occupy fixed, standardized positions with respect to the silicon carrier and gold shell. If the location and orientation of the plaque is known, precise seed coordinates can be derived from a model of the plaque's structure. A plaque data file identifies the location, length, orientation and contents (I-125, Ir-192, or empty) of slots into which sealed sources can be loaded, and the radius of the sphere (plaqRadius in Fig. 3) to which the plaque conforms. The origin of the plaque's coordinate system is the center of this sphere. Three angles define the orientation and displacement of each source from a standard orientation and position. Referring to Figs 2 and 3, the standard position is defined as x = -(plaqRadius + seedOffset), y = 0, z = 0. The standard orientation has the long axis of the source parallel to the z-axis (seedTilt = 0°). The seed is first rotated about the x-axis by seedTilt, then about the y-axis by seed α, and finally rotated about the x-axis once again by seed β. A plaque description also includes the thickness of the plaque on the central axis (caxHeight), the location of suture eyelets, and a table of 24 radii which approximate the perimeter of the gold shell. The angular interval between radii is typically 15', although they may be distributed irregularly if desired. A plaque file is created by measuring the plaque parameters and writing a computer program to create the plaque file algorithmically, by digitizing the plaque outline and slots from photographic frontal views, and/or by editing an existing plaque using interactive graphics.
|
Fig. 3. Lateral view of the plaque coordinate system. A slot is initialized with its geometrical center at a standard position (x = -(plaqRadius + seedOffset), y = 0, z = 0) and oriented with its long axis parallel to the z-axis (seedTilt = 0°).
|
A plaque description can be modified by changing the isotope loading pattern or the appearance of the plaque itself. A plaque editing window provides an expanded frontal view of the plaque in an interactive graphics mode. The mouse and screen pointer are used to install or remove seeds from a slot by pointing at the slot and "clicking" the mouse button. Standard default settings for isotope, source activity, implant duration, and other plaque related parameters are modified from "pull-down" menus and dialog windows, and may be overridden for individual seeds. Any combination of source activity and type is permitted. In addition, patterns of slots may be added or removed from the plaque and slot positions moved to new locations on the plaque using the interactive graphics interface. The plaque perimeter can be modified to indicate asymmetrical characteristics such as notches and suture eyelets. The modified plaque can be renamed and saved to disk for future use. The interactive editing capability permits custom plaque descriptions to be rapidly created from a library of previous patients and plaque designs.
Positioning the plaque on the eye
|
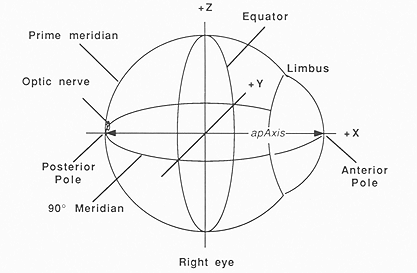
Fig. 4. The coordinate system used to indicate location on the surface of the eye. Latitude and longitude are specified with respect to the equator and prime meridean. The prime meridian begins at the posterior pole and passes through the positive z-axis. The positive y-axis is directed "away" from the viewer.
|
The position of the plaque during treatment is defined using a spherical, solid surface, 3D perspective projection of the eye. Left or right eye, anterior to posterior pole length (apAxis, Fig. 4), the diameter of the limbus and equator, and other ocular dimensions obtained from CT, MRI, ultrasound and/or direct caliper measurement are specified from menus and interactive dialogs. The eye, and markers for anatomical structures such as optic nerve are then dimensionally scaled to these parameters using the size and anatomic descriptions of Newell (19), Last (13), and the COMS. Displays for anterior, posterior, medial, lateral, superior or inferior views, as well as free rotation in three dimensions may be selected from a menu. To achieve the display speed necessary for smooth animation, the eye is drawn as a wire frame outline without hidden line removal during free rotation. Calculating and redrawing the solid-surface display requires about 2 seconds, which is too slow for animation. A "zoom" feature allows magnification of the screen image by up to 5 times to facilitate precise positioning of the plaque. The position of the geometrical center of a plaque during treatment is specified by "grabbing" the image of the plaque on the screen using the mouse controlled screen pointer, and "dragging" an animated, 3D wire frame outline of the plaque to the desired location. Alternatively, the plaque can be automatically centered over the tumor. The rotational orientation of the plaque with respect to its central axis is also specified interactively or from a dialog window.
|
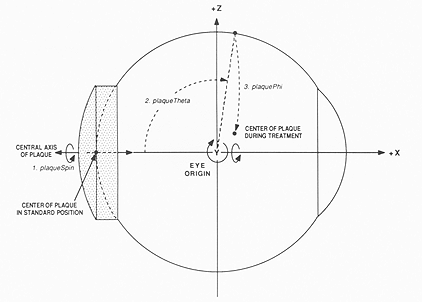
Fig. 5. Lateral view of the eye coordinate system. Although the operator of the program uses the more familiar terms of latitude and longitude to describe the plaque position, within the program the position and orientation of the plaque is handled as a sequence of angular displacements from the standard position in the local coordinate system of the eye. The plaque is first spun about its own central axis (plaqueSpin) to account for orientation, then rotated about the y-axis (plaqueTheta), and finally rotated about the x-axis once again (plaquePhi) to bring its center to the desired position.
|
Within the program, the position and orientation of the plaque are handled in a manner similar to that used to describe seed locations within a plaque. The plaque is initialized in a standard geometrical position and orientation with its center at the posterior pole of the eye. Figure 4 illustrates the location of the poles, equator, limbus, and meridians with respect to the anatomy of the eye. The latitude and longitude of the plaque center, and the orientation of the plaque during treatment are converted into a sequence of rotations from the standard position (in the local coordinate system of the eye). Referring to Figure 5, the plaque is first spun about its own central axis (plaqueSpin) to account for orientation. In the standard geometry, the central axis of the plaque is the same as the x-axis of the eye, so this involves a rotation about the x-axis. The plaque is then rotated about the y-axis (plaqueTheta), and finally rotated about the x-axis once again (plaquePhi) to bring its center to the desired position.
Calculating and displaying the dose distribution
Transverse, saggittal, or coronal planar cross-sections may be requested, as well as any plane transecting the eye diametrically. These planar surfaces are displayed within a translucent eye. In addition, any spherical surface within or surrounding the eye can be displayed as a 3-dimensional perspective projection or as a funduscopic (or "retinal") diagram. Interactive zoom and pan on the dosimetry surface is provided. Dose calculation matrices ranging from 20 X 20 to 160 X 160 points may be selected. The matrix may be applied to a planar dosimetry surface in any rectangular subregion ranging from 2 to 40 mm on edge. Bilinear interpolation is used to estimate isodose contours between the calculated points. A variety of color and grey scale isodose display options are provided including a library of predefined formats covering one to four orders of magnitude. User definable formats are also available. The display can be normalized to the dose at any location on the central axis of the plaque or the apex of the tumor. Alternatively, the dose at any point on the dosimetry surface can be calculated explicitly and displayed numerically by "clicking" the pointer at the location. A table of dose values at I mm intervals on the central axis of the plaque, and to the center of certain ocular structures is also available.
The dosimetry algorithm initially treats each seed as an unfiltered line source, located on the longitudinal axis of the physical seed, in a full scatter geometry. Various dose modifying factors, taken from the literature and from our own measurements are then applied to account for tissue attenuation and scatter (15), angular anisotropy (14, 25), and deviation from full scatter geometry due to the gold shell (18). The activity of each source at the start of treatment is specified in the plaque description. Although the program defaults to a 1 hr calculation, any calculation period may be specified. Source decay is automatically included in the calculation. For sources which are offset from the scleral surface, the intervening medium is presumed to be tissue equivalent. The dose calculation model has been described previously, and compared to TLD measurements in an acrylic phantom (17).
|
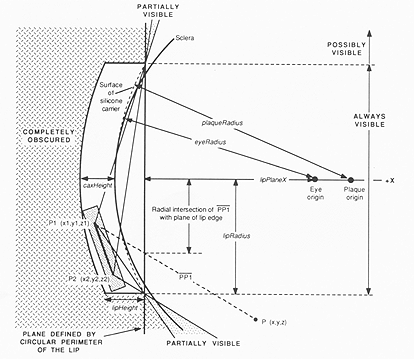
Fig. 6. Diagram of the standard geometry for plaques with a circular lip. This standard geometry simplifies the calculation of what portion of a seed is visible from an arbitrary position P in 3-dimensional space. See text for explanation.
|
Collimation of the direct photon fluence from each source by the lip of a plaque with a circular perimeter (any of the COMS plaques) is accounted for by considering the plaque to be in the standard geometry discussed above. Instead of rotating the plaque and its sources, the calculation point is rotated by the inverse transformation, bringing it to a corresponding location in the standard geometry. In the standard coordinate system, if the x coordinate of the rotated dosimetry point P (x, y, z) falls "behind" the plane defined by the circular perimeter of the plaque (x <= -lipPlaneX in Fig. 6) then the position of P is compared to the structure of the gold shell. If P lies outside the cylinder defined by the lip (i.e., (y² + z²) > lipRadius²) or if P lies within the cylinder and behind the plaque (i.e. (x < 0) and (((x + eyeRadius - plaqRadius)² + y² + z²) > (plaqRadius + caxHeight)²)) then the sources are completely obscured by the gold shell and the dose is modified by the transmission factor (for the particular isotope) through the gold. For I-125, the transmission is considered to be zero.
If the x coordinate of P lies in front of the plaque (x > -lipPlaneX) and P lies within the cylinder defined by the lip, then the sources are always in direct sight, and the gold shell has no direct effect. If P lies outside the cylinder, then the intersections of lines between P and the endpoints of the seed (PPI and PP2) with the plane x = -lipPlaneX are calculated. Lines which intersect this plane within the circular perimeter of the lip indicate that the endpoint is visible from P, whereas lines which intersect outside the circle indicate an endpoint which is obscured by the lip. If both end points of a source are visible there is no lip attenuation. If both endpoints are obscured, the gold transmission factor is applied. If one endpoint is visible and the other is obscured, the source is partially visible and an iterative procedure is used to estimate the "partial visibility ratio" (pvr = visible length / source length). The gold transmission factor is applied only to the portion of the seed which is obscured. An iterative algorithm was chosen to estimate the pvr in order to reduce computational complexity. The dosimetry algorithms are available from the author.
The lip calculation currently considers only the primary photon flux from a source. Luxton et al (17) have observed that backscatter from an eye phantom shielded by a plaque is about 3% of the unshielded exposure rate. This suggests that scatter into shielded regions away from the penumbral region is not of great clinical significance. The relative contribution of scatter to the penumbral region, however, is unknown. At this time we must consider that our calculation underestimates dose in the penumbral region.
Abstract |
Results |
Discussion & References





